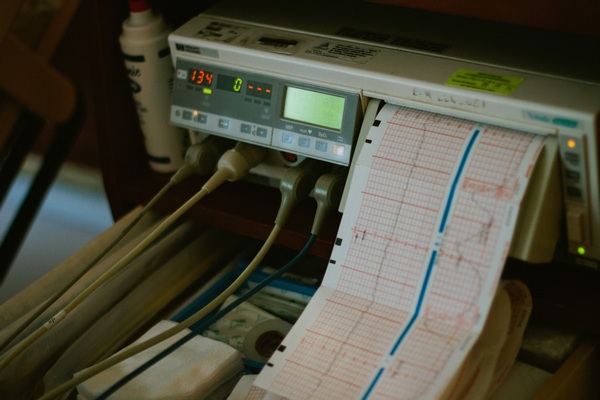
Have you ever felt that your heart beat was not normal? If you do feel that your heart beat was “different” from your usual heart beat rhythm, you should check your pulse at your wrist and ask yourself whether the pulse rate is fast and whether it is regular. If your pulse rate is transiently faster than 120 beats per minute when you are at rest or is irregular in rhythm, it is best you see your doctor for an opinion. As life span increases, the likelihood of developing an abnormal heart rhythm or arrhythmia increases as age increases. Some of these arrhythmias may be harbingers of death and should not be taken lightly.
Death from atrial fibrillation
The commonest type of arrhythmia is atrial fibrillation (AF). In AF, the upper heart chamber (atrium or atria for plural) is beating at the rate of about 400 beats per minute. Instead of the electrical impulse of the heart being generated from the pacemaker at the right upper chamber, this haphazard abnormal AF electrical impulse usually originates in and around the sites where the lung veins (pulmonary veins) join the left atrium. There are usually 2 pulmonary veins from each lung which carry oxygenated blood from the lung into the heart chamber. Not all the AF electrical impulses that are generated are transmitted through the heart electrical circuits to the lower pumping chambers of the heart (ventricles) and the intermittent transmission results in varying heart rates and therefore an irregular heartbeat. The AF is usually intermittent, lasting second to minutes, but over time can become prolonged in period and become permanent.
As the atria are virtually just ”quivering” in AF, blood flowing into the left atrium from the pulmonary veins will slow down and even “stagnate” in the part of the left atrium called the atrial appendage which is an outpouching with a blind end. There is a high risk of blood clot formation in the left atrial appendage and if the blood clot becomes loose and flows out of the heart chambers into the aorta and the neck arteries into the brain, a massive stroke can occur. AF also causes atrial enlargement and heart failure. Data from the United States Centres for Disease Control shows that the death rate from AF as the primary or a contributing cause of death has been rising for more than two decades.
Incidence of atrial fibrillation
In the 2014 American College of Cardiology guidelines for the management of atrial fibrillation, it is estimated that about 9% of those whose age is 65 years or more have AF. In a longitudinal 21 year study on a population in the United States by Yoko Miyasaka from Mayo Clinic which was published in the Circulation journal in 2006, it was estimated that for every 100 males followed over a 10 year period, about 13% have AF for those age 65 to 74 years increasing to about 40% in those 85 years or more. For women, the incidence was lower, with about 7% having AF for those age 65 to 74 years increasing to about 28% in those 85 years or more. In a recent publication in Circulation journal, investigators of the ASSERT-II trial found that as high as about 30% of the asymptomatic patients 65 years or more, with risk factors for heart disease and stroke but with no prior stroke, had AF.
This means that those who are 65 years of age or more must be on the alert for AF especially if they have risk factors for heart disease or stroke. The risk is even higher if the left atrium is enlarged.
Reducing the risk of atrial fibrillation
Given that AF is highly prevalent with increasing age and is associated with an increased risk of disabling stroke and death, it can only be meaningful to understand the factors that will increase the risk of stroke and take active measures to reduce this risk.
What are the risk factors that predict an increased risk of AF? One of my relatives presented with a sudden massive stroke which was diagnosed to be due to a large blood clot arising from the left atrium.
He had AF due to excessive thyroid hormones which he was not even aware of. Fortunately, rapid intervention resulted in subsequent resolution of the stroke and treatment of his thyroid condition resulted in complete resolution of the AF. Another recent patient of mine who developed heart failure and AF had excessively high thyroid hormones which were beyond the upper range of measurement. Successful treatment of the thyroid condition resulted in resolution of the heart failure and AF. For patients with weight loss, frequent palpitations, hand tremors and persistent warm sensation, blood tests should be performed to look for elevation of the thyroid hormones. This is one of the most easily preventable causes of AF.
High blood pressure is the most commonly attributable cause of AF in the population and good control of AF can prevent the onset of AF. Poorly controlled blood pressure results in a higher pressure in the left atrium. As the left atrium has a thin wall, increased pressure will result in swelling of the left atrium and disruption of the “electrical system” in the atrial wall and pulmonary veins. This electrical instability will cause abnormal heart impulses to fire off spontaneously from around the region of the left atrium and pulmonary vein, resulting in AF.
The next commonest attributable cause of AF is obesity and weight loss surgery such as bariatric surgery have been shown to reduce the incidence of AF. Significant weight reduction of at least 20% has been shown to be effective in AF reduction.
Lifestyle factors such as excessive alcohol consumption and smoking are risk factors for AF which can be modified by cessation of these habits. For those who engage in frequent high-intensity endurance training, the risk of AF is also increased. Sleep apnoea has also been found to be associated with AF.
Disease of the heart resulting in heart failure, significant blockage of the heart arteries and disease of the heart valves are also risk factors for AF. The presence of diabetes mellitus is also a risk factor for AF as it can predispose to narrowing of heart arteries. Procedures such as open heart artery surgery can result in AF in the immediate post-operative period but most of these patients have complete resolution of the AF within a few weeks.
Based on the most recent data, most of the causes of AF are potentially modifiable and genetic causes of AF account for less than 2% of the cases of AF.
Preventive approach for AF
Frequent paroxysmal AF or permanent AF often requires long term blood thinners to prevent stroke but long term consumption of anticoagulation is associated with bleeding complications. Based on a publication in Stroke in August 2017 by Craig, the risk of brain bleeding ranges from 1.6 events to 6.1 events for every 1000 patients every year on anticoagulants. Medication for AF is unable to cure the condition in most situations and will require lifelong medication. Even then, the condition will continue to progress over time.
Insertion of special catheters into the left atrium to “burn” a closed ring around the entry point of the pulmonary veins in an attempt to “isolate” the source of the abnormal heart rhythm and prevent it from spreading to other parts of the heart is used to treat the problem. However, the recurrence rate is high and the exposure to X-ray radiation is also high.
Hence the best approach to AF is to identify those with risk factors and take preventive measures. In the case of AF, the old adage holds true – Prevention is better than cure.